|
Materstvedt then argues that euthanasia ‘ends’ rather than ‘relieves’ suffering, and by virtue of this it does not constitute a treatment per se, rendering my original arguments a non-starter. I therefore do not think that my research ought to contribute to opiophobia or have harmful real-world consequences. By arguing that there may not be an ethically-significant difference between palliative opioid and sedative use and euthanasia, I have been attempting to advance the case for the latter rather than hinder the case for the former. 
I have treated many dying patients in both general hospitals and hospices, and know how essential they are in achieving adequate pain and other symptom relief. I would also like to emphasise that I wholly and passionately advocate for the use of opioids and sedatives in the palliative care setting. The Australian and New Zealand Society of Palliative Medicine also aligns itself with this policy. Furthermore, in my personal clinical experience, CDPS does not fall beyond the scope of routine palliative care, and this is supported by the European Association for Palliative Care’s framework on palliative sedation which was introduced by Schofield et al. Based on the current level of information available, a position of agnosticism regarding whether they hasten death in this setting is still appropriate. However, it is well known that one drug can have varying effects when used in different clinical settings, and I argue that the paucity of evidence regarding opioid and sedative safety in the specific palliative care population is highly relevant and problematic. 
They also argue that continuous deep palliative sedation (CDPS), a subset of palliative sedation, falls beyond the scope of routine palliative care, and that my research will contribute to opiophobia and be deleterious to the provision of palliative care globally, and therefore be harmful to patients, their families and health professionals. correctly acknowledge that there is a wealth of information showing that opioid and sedative use is safe in other settings outside of palliative care, and then argue that I have introduced a cherry-picking bias by focusing solely on the palliative care population. In my original essay I conducted a literature search which found that there is not a strong body of evidence supporting this claim, suggesting that we should adopt a position of agnosticism on the matter. I can clearly recall from my medical student days being constantly taught (and reassured) that opioids and sedatives, when appropriately used in the palliative care setting, do not hasten death, and that they are therefore far removed from euthanasia. 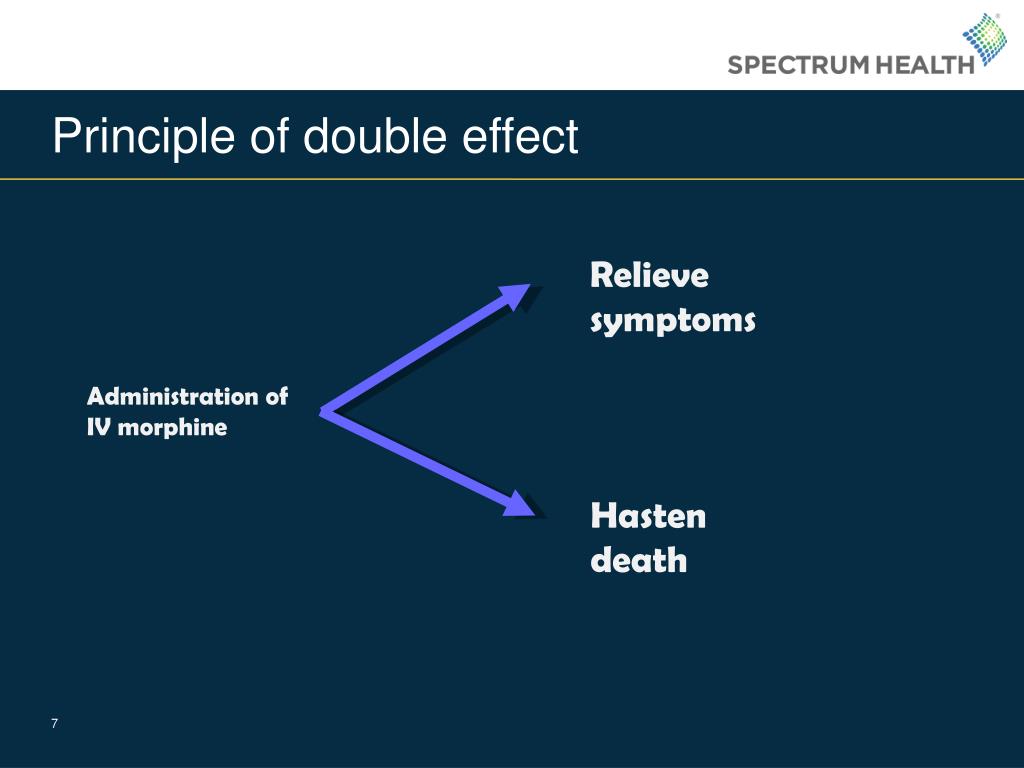
I will briefly comment on some of these points here. One of my recent essays has generated a considerable amount of critique which I was fortunate to be able to explore in my essay ‘A response to critics: Weakening the ethical distinction between euthanasia, palliative opioid use and palliative sedation’.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
